AJIMSHAW’s Approach part III
SPECIFIC SESSIONS
II. Internal Pelvic Release
Fascial tightness of the perineum and its structures have major role in pelvic floor dysfunction and pain. Inorder to balance the pelvic floor it should be managed both externally and internally. This session explains the techniques of ‘Internal Pelvic Release’.
To understand the importance of ‘Internal Pelvic Release, have a look at the below picture. The “X” marked are trigger points in pelvic floor muscles and the reddish areas are the referred pain due to the trigger points. ‘Internal Pelvic Release’ is the most advanced way to release these triggerpoints.

60-80% DID NOT RECEIVE AN ACCURATE DIAGNOSIS (GPWPP 2007)
Causes of Pelvic Myofascial Trigger Points
Excessive tension on muscle fibers
Straining
Habitual tightening
Trauma as in pregnancy, injury
Inflammation
Types of Pelvic Floor Muscle Trauma
Severe trauma from accidents of falls (coccygeal injury)
Urological or gynecological surgery
Repetitive minor trauma from bicycle seats, uncomfortable chairs
Childbirth
Inflammation of the Pelvic Organs
Infections eg:- prostate, bladder, vaginal
Endometriosis
Inflammatory bowel disease/IBS
Feet position and Pelvic Dysfunction

Correct your Foot deformity and improve your pelvic floor function!
THE PERINEUM
 The perineum and perineal body lies between the vagina and the anus on a female and between the bulb of the penis and the anus on a male. The Perineal body is essential for the integrity of the pelvic floor, particularly in females. Its rupture during delivery leads to widening of the gap between the anterior free borders of Levator Ani muscle (pelvic floor muscles) of both sides, thus predisposing the woman to prolapse of the uterus, rectum, or even the urinary bladder.
The perineum and perineal body lies between the vagina and the anus on a female and between the bulb of the penis and the anus on a male. The Perineal body is essential for the integrity of the pelvic floor, particularly in females. Its rupture during delivery leads to widening of the gap between the anterior free borders of Levator Ani muscle (pelvic floor muscles) of both sides, thus predisposing the woman to prolapse of the uterus, rectum, or even the urinary bladder.The following muscles converge and are attached to the perineum:
External anal sphincter
Bulbospongiosus
Superficial transverse perineal muscle
Anterior fibers of the levator ani
fibers from external urinary sphincter
Deep transverse perineal muscle
Because of different reasons myofascial dysfunctions and trigger point developments are very common and most of the time these trigger points will be unidentified and its importance is being ignored. Result; increasing pelvic floor dysfunctions and pain.
As we have discussed in the previous sessions the success of ‘Self Myofascial Release’ lies in the ability of finding the exact sites of myofascial restrictions and trigger points. Palpation with your finger tips and application of firm pressure over 90 seconds is the basics of SMFR.

The picture illustrates the techniques of palpation of myofascial restrictions and trigger points. When you reach the restricted area you can find or feel nodules, bands or thickness. Pressure on this area will produce pain over there and you will feel pain radiating to adjacent or distant areas which is called radiating pain.
Trigger points in the perineum and vulva.
The picture below is a true representation of myofascial restrictions and trigger points in the perineal area and the vulva(female external genitalia) the ‘blue’ shades represents triggerpoints which can be approached externally and ‘yellow’ shades represents triggerpoints which only be approached internally. Every person’s myofascial restriction patterns and dysfunctions vary. You have to examine each of this area using the below picture as reference. On palpation if you feel pain marks that area with a non irritant marker.
 Vulva with triggerpoints
Vulva with triggerpoints(Save this picture or take a print out for reference during SMFR)
Common Sites of Connective Tissue Restrictions in pelvis

Perineal SMFR is a technique which slowly and gently releases the myofascial trigger points and restrictions around the vagina, perineum and rectum.
CAUTIONS:
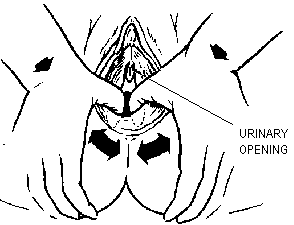
Avoid the urinary opening (see diagram) to prevent urinary tract infections.
Do NOT do Perineal SMFR if you have active herpes lesions or any other infections, as you could spread the infection to other areas.
General Hints:
The first few times it’s helpful to use a mirror to find the vagina and perineum and see what they look like.
If you feel tense, take a warm bath or use warm compresses on your perineum for 5 to 10 minutes.
If you have had an episiotomy with a previous birth, concentrate part of your SMFR on that area, Scar tissue isn’t as stretchy as the rest of your skin and needs extra attention.
After Perineal SMFR, tone up the muscles in the vagina by practicing the pelvic floor (Kegel) exercises regularly.
Directions:
1. Wash your hands.

2. Find a private, comfortable place and sit or lean back in a comfortable position.
 3. Put a lubricant such as KY Jelly, vitamin E oil, or pure vegetable oil on your thumbs and around the perineum if the skin is very dry/ scaly. Care should be taken for extra hygiene and use lubricant in a lesser quantity. For Perineal SMFR you can use the tools which we have discussed earlier (nobbers, myoballs etc)
3. Put a lubricant such as KY Jelly, vitamin E oil, or pure vegetable oil on your thumbs and around the perineum if the skin is very dry/ scaly. Care should be taken for extra hygiene and use lubricant in a lesser quantity. For Perineal SMFR you can use the tools which we have discussed earlier (nobbers, myoballs etc)
4. a. Pelvic diaphragm Release
Use the below description if your partner or care giver can help you other ways apply pressure over the prescribed area by using appropriate tools.

 • Lie on your back in a comfortable position
• Lie on your back in a comfortable position• Let your partner to sit at side of pelvis to be treated, facing your head
• Bend your knee and hip and introduce index & middle fingers medial to ischial tuberosity (the ischiorectal fossa)[when you are palpating the area as shown in the picture above you can feel a bony prominence over there]
• Take a deep inspiration and during exhalation, press fingertips superiorly as shown I the picture in a slow and sinking way.
• Maintain this position, during next exhalation, continue to follow and press fingers more superiorly (and deeply)
• Repeat several cycles
• RE-TEST
• Alternately you can use myo balls, nobbers etc for this release.
4.b. Perineal SMFR
Trigger points (which cause referred pain in persons with chronic pelvic pain/ic) in the perineum can refer pain and sensation to the rectum, vagina, and site of palpation. It is very important that you have to release this area by SMFR.
Apply pressure to the perineal body ----the technique is far gentler, for the tissue and muscles here can be very sensitive. Take it easy when applying pressure to perineal body; find out the restrictions and trigger points, apply pressure and gradually sink into the area, hold there for 90 second time, concentrate on your breathing, try to sink down during deep exhalation. Treat multiple areas as necessary. Remember you are trying to soothe pain, feed the area blood and oxygen, not beat it into submission.
You will need either of a comfortable tool as we mentioned earlier. If you don't have one apply pressure using finger tips or a dilator until you can purchase one. It is important that you find a comfortable place to lay down where you will be ensured privacy.(Note: perineal SMFR is especially helpful before and after sexual activity.)If you use gloves they should be non-latex and lubricants should be paraben-free and have no propylene glycol which can irritate the tissue. Check labels.

4. c. Vulvar SMFR
The SMFR procedure for the vulva is same as for other SMFR. But in vulva you have to check for restrictions in a systematic manner. There can be inactive or multiple fascial restrictions. So palpate areas by dividing it into multiple sections (refer the trigger point diagram above and compare)
4. d. Vaginal SMFR
For vaginal SMFR a clean hand with or without a sterile glove is enough. Our goal is stretching the pelvic floor muscles through either vagina or rectum. Use your finger (index finger, some finds comfort by using both the thumbs together for the opposite sides, select as per your convenience)
Stretch the vaginal wall with an aim to go deep and find out the restrictions at the internal pelvic floor muscle. We used to call his as “Palpation through stretching” move around the vagina while maintaining the stretch, apply firm pressure to the restrictions or trigger points for 90 seconds and repeat the treatment.
This treatment is especially useful for all type of female genital discomforts and pain especially after the menopause.
Follow the pictures

 Home program for painful intercourse
Home program for painful intercourse
 SELF TREATMENT: URGENCY/ FREQUENCY
SELF TREATMENT: URGENCY/ FREQUENCY

Use the picture “Vulva with trigger” point as reference
4. e. Rectal SMFR
Rectal SMFR is indicated for those females who are having chronic pelvic/sacral/coccygeal pains and for males. The techniques of application is same like the ‘vaginal SMFR” provided that a sterile glove should be used always. Most of the clients finds it difficult , but the difficulty depends on your physique. A partner can help you in this regards.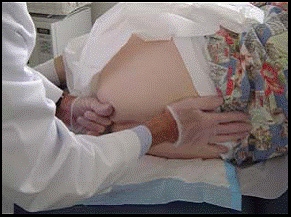


SUMMERY
Success in the management of all painful pelvic, gynecological conditions needs multidisciplinary approach. You need to remain active. Performing some back exercises and pelvic floor exercises immediately after the release is found to hasten the improvement. So be active and be cool. Don’t forget that there will be an increase in discomfort when you are starting the SMFR, don’t give up it’s a short period after that you will praise me.
My advice is be cool, be active and be a master of pelvic SMFR. If you are having any queries please contact me via scebcaptmfr@gmail.com.
Joining/ making pelvic pain interest groups are always good. So plan for that too. Discuss these topics among you. Please inform other pelvic floor dysfunction patients about this.
2 comments:
My physique does not allow me to do the self rectal myofacial release that I require. What are the appropriate tools you mention & where can I obtain them? Also, how are they properly used. I am a woman with pelvic floor, coccygeal & neurogenic bladder issues as well as rectal incontinence & pain.
ok
Post a Comment